- Home
- >
- About Psychosis
- >
- Signs and Symptoms

The term “psychosis” describes conditions that affect the mind, causing a loss of contact with reality or trouble deciding what is real and what is not. Psychosis can change a person’s thoughts, feelings, and behaviours. Periods when symptoms are more intense or frequent are called episodes.

Common symptoms of psychosis feel very real and include hallucinations, delusions (false beliefs), paranoia, or disorganized thoughts and speech. Other symptoms may include:
-
A significant change in “normal” personality or mood for a sustained period of time.
-
Changes in body movements, restlessness, or agitation.
-
Severe changes in sleep patterns or sleep disturbances.
-
Preoccupation with strange or unusual ideas.
-
Overpersonalizing events, songs, TV, and social media (having special meaning directed to the individual).
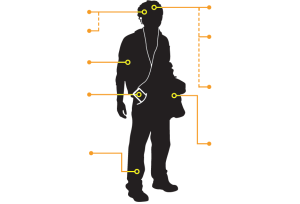
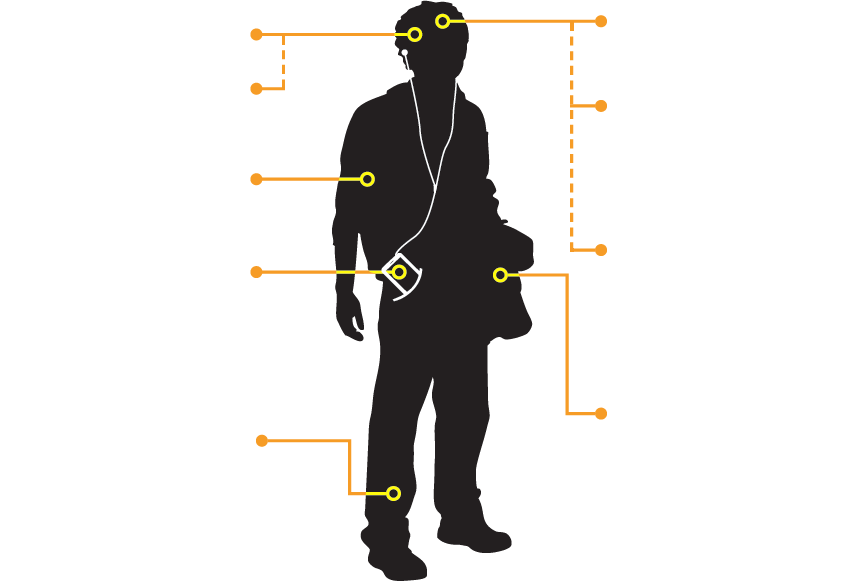
For more information, view the “Anatomy of Psychosis” information sheet, below.
“Early psychosis” or “first episode psychosis” means someone is experiencing psychosis for the first time. An estimated 3% of people will experience a psychotic episode at least once in their life.
Evidence shows that some forms of psychosis have to do with dysfunction in the brain’s neurotransmitters and/or genetics. Psychotic episodes can also be triggered by stress or by substance use.
The duration of an episode varies and depends on the person. It could be a few hours or days up to months or years without proper treatment or support. Most first episodes occur in the teen years or early adulthood.
Identifying and treating psychosis early can aid recovery and reduce duration, need for medication, and hospital stays.
This is particularly important for teenagers and young adults, because psychosis can disrupt relationships, work, and schooling, which can lead to additional problems—such as isolation, unemployment, substance abuse, depression, self-harm, or suicidal thoughts.
 What is Psychosis?
What is Psychosis?
Download the printable information sheet:
English | French | Italian | Spanish | Chinese (Mandarin) | Portuguese | Punjabi